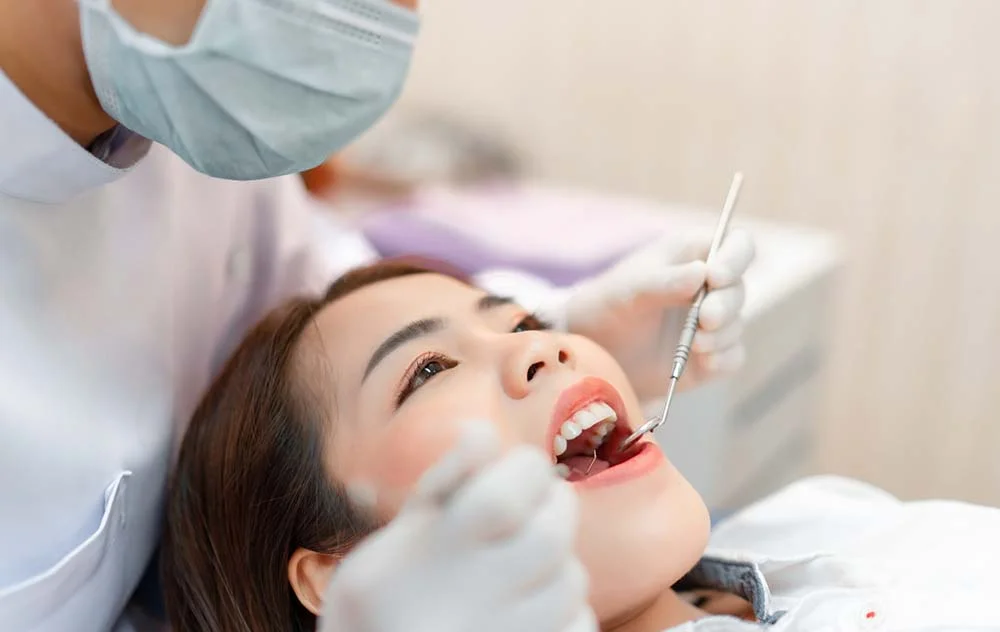
Policy Statement on the Role of Dentistry in the Treatment of Sleep Related Breathing Disorders
Sleep related breathing disorders (SRBD) are disorders characterized by disruptions in normal breathing patterns. SRBDs are potentially serious medical conditions caused by anatomical airway collapse and altered respiratory control mechanisms. Common SRBDs include snoring, upper airway resistance syndrome (UARS) and obstructive sleep apnea (OSA). OSA has been associated with metabolic, cardiovascular, respiratory, dental and other […]
We are featured in Dental Asia
Dental sleep experts unite at the 2nd Asia Pacific Dental Sleep Medicine Fellowship Day
The Relationship Between Primary Sleep Disorders and Temporomandibular Disorders
Background: While evidence is accumulating to propose a specific contribution of sleep disorders and low quality sleep in the pathogenesis of temporomandibular disorders (TMD), management of primary sleep disorders in the process of preventing and treating TMD still remains scientifically unsupported. Objective: To investigate the association of primary sleep disorders with TMD risk in South Korea. Patients […]
APAC Set to Propel Sleep Apnea Device Market Growth: Report
The Asia-Pacific (APAC) region is poised to significantly drive the growth of the sleep apnea device market over the next five to ten years, according to a report by MarketsandMarkets. Key factors contributing to this growth include the expansion of leading industry players into emerging markets such as India, Australia, the UAE, and Saudi Arabia. […]
Inspire Recalls Key Component of Neurostimulator Therapy for OSA
The recall addresses a defect in the Inspire IV implantable pulse generator that may cause malfunctions and necessitate revision surgery for patients. Summary: Inspire Medical Systems has issued a recall for its Inspire IV implantable pulse generator used in treating obstructive sleep apnea due to a manufacturing defect. This defect may cause system malfunctions, including […]
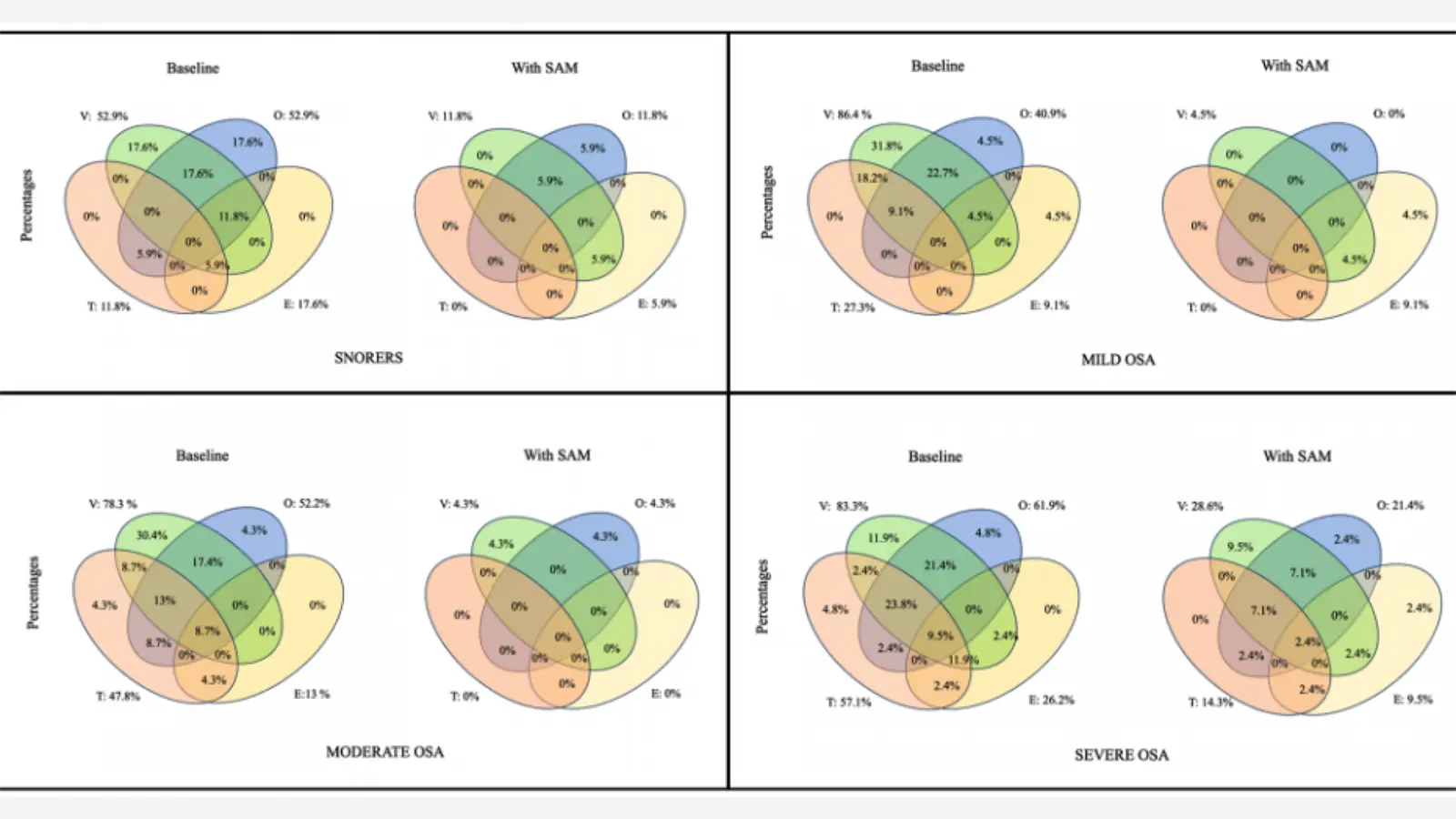
Modifications in Upper Airway Collapsibility during Sleep Endoscopy with a Mandibular Positioner
Abstract Background: Mandibular advancement devices (MADs) are an effective treatment for patients with sleep-related breathing disorders, with variable response. Increasingly more research points to the predictive value of Drug-Induced Sleep Endoscopy (DISE) in patient selection. This study aims to analyze the changes in upper airway collapsibility using a titratable MAD simulator during DISE. Methods: This […]